Infection removal
The infected pulp is removed and the inner chamber is cleaned so bacteria are no longer trapped inside the tooth.
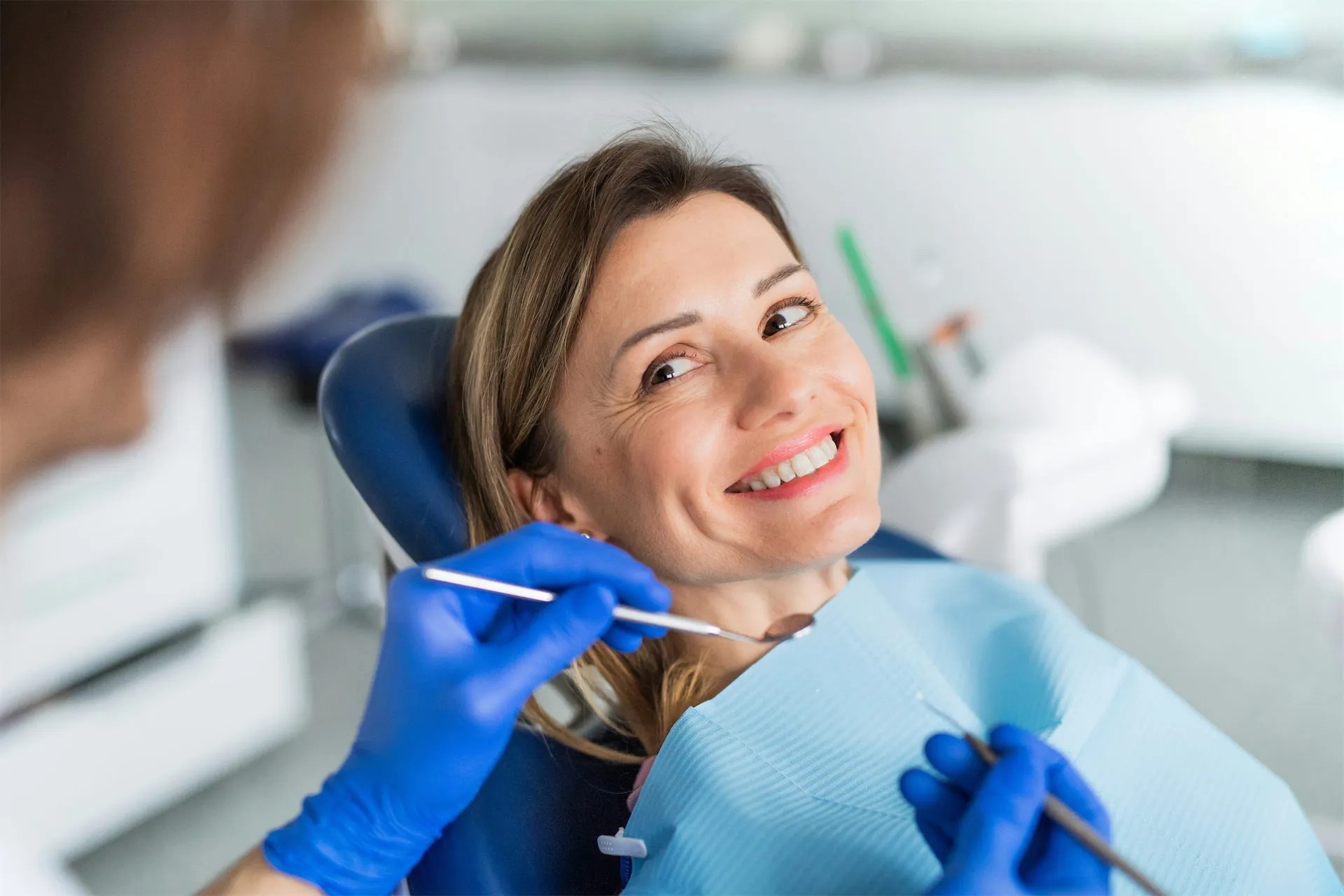
Root canal therapy treats infection inside a tooth and can often save it from extraction while relieving pain and inflammation.
Save An Infected Tooth
When decay or trauma reaches the pulp inside a tooth, the nerve and blood vessel tissue can become inflamed or infected. Root canal therapy is the treatment used to remove that infected material, disinfect the inside of the tooth, and seal it so it can continue functioning.
The source material for this page made two points worth keeping: root canal treatment is used when the inside of a tooth becomes infected, and the procedure itself is not the painful part. In most cases, the infection is what causes the pain. Root canal therapy is the treatment that removes that source of discomfort.
Teeth usually need root canal therapy for one of two reasons. Deep decay can progress through the enamel and dentin until bacteria reach the pulp, or a crack or traumatic injury can expose the inside of the tooth. Symptoms often include persistent toothache, temperature sensitivity, tenderness when chewing, or swelling around the gums.
Saving the natural tooth is often preferable when it can be done predictably. Root canal therapy allows that by eliminating infection while preserving the remaining tooth structure for restoration.
Why It Matters
The goal is not just to stop pain. It is to remove infection while giving the tooth a chance to remain functional.
The infected pulp is removed and the inner chamber is cleaned so bacteria are no longer trapped inside the tooth.
Treatment addresses the source of severe tooth pain rather than only masking symptoms.
When successful, root canal therapy allows you to keep the natural tooth instead of moving directly to extraction.
After the root canal, the tooth can usually be rebuilt with a filling or crown to protect it long term.
Modern Endodontic Care
A common misconception is that root canal therapy is unusually painful. In reality, modern treatment is designed to make the procedure manageable and to eliminate the pain caused by infection.
During treatment, the tooth is numbed, isolated, and opened so the damaged pulp can be removed. The interior of the tooth is then cleaned, shaped, and disinfected before being filled and sealed. In many cases, the final step is a restoration that protects the tooth from fracture.
Molars and premolars are often restored with crowns because they handle more chewing force. Some front teeth can be restored with fillings if enough healthy structure remains. The right restoration depends on the location and condition of the tooth.
Treatment Flow
The exact sequence can vary, but most root canal treatment follows a predictable pattern from diagnosis to final restoration.
Your dentist evaluates symptoms, takes X-rays when needed, and confirms whether the pulp is inflamed or infected.
The tooth is anesthetized and opened so the inner nerve tissue can be reached safely and comfortably.
The infected pulp is removed, the inner canals are disinfected, and the space is sealed to prevent reinfection.
A filling or crown is used afterward to protect the tooth and return it to function.
FAQ
These are the concerns most patients want answered before deciding whether root canal treatment is the right step.